The Healthcare (R)evolution
Membership required
Membership is now required to use this feature. To learn more:
View Membership BenefitsWhy now?
I turned 62 over the summer and have to admit – whether willingly or unwillingly – that I have had a few ups and downs over the years, health-wise, with the most life-changing incident being the near-fatal bicycle accident I had in 2014. In the years since the accident, healthcare has formed a big part of my life, and I wasn’t hard to convince when Rishanth (the newest member of our research team) came to me over the summer and suggested he allocate some serious time to the topic.
As he said: “We have identified six megatrends that drive our thinking and our portfolio construction. Do you realise that healthcare spending will be affected by at least two of those six megatrends?”. The short answer is, yes, I do realise, but sometimes we all ignore the obvious. Thank you for reminding me, Rish.
The problem I have been up against after taking on this project is that healthcare is a monumental topic. Where do I start and when do I draw a line in the sand? If you think I only scratch the surface in the following, I can only apologise, but none of us want to sit here for the next 18 months. Having said that, Rish is only a phone call away (+44 8939 2909), should you want to talk to him about investment opportunities in the healthcare universe – topics I am not supposed to write about in the Absolute Return Letter.
Having said that, I can assure our ARP+ subscribers that the September Absolute Return Letter, which you are holding in your hands now, will be followed up with a research paper on the same topic. That paper will provide much more information on investment opportunities in the healthcare space.
More insight, more advice, more in-depth.

The big picture
Although society is getting older, many observers continue to argue that the impact in the short to medium term will be minimal – it is such a slow-moving wave, they argue. I guess it depends on how you define “short to medium term”. If “short term” means the next few weeks and “medium term” takes us to Christmas, it is hard to disagree with that observation. However, if “short term” is the next year or two and “medium term” is the next handful of years, as it is in my book, then it would be a massive mistake to underestimate the impact on society from changing demographics.
As you can see in Exhibit 1 below, between now and 2035, the working age populations of Germany and Italy - two of the biggest countries on the European continent – will shrink by about 10%, and so will the working age population of Japan. So many people will retire over the next 15 years in those three countries, and the younger generations are not big enough to fill their shoes.
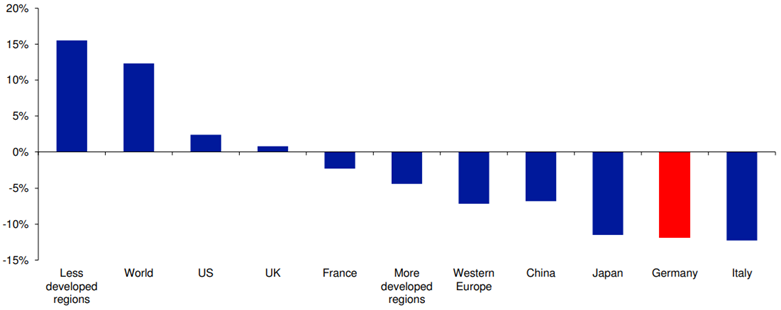
Note: Selected countries and regions
Source: Deutsche Bank Research, Haver Analytics
Many countries were not included in the work conducted by Deutsche Bank Research, but I can assure you that Germany, Italy and Japan are not even the worst affected countries – not at all. In Asia, South Korea stands out as the dubious ‘winner’, and most Eastern European countries make the numbers in Germany and Italy look like a rounding error.
In the context of healthcare spending, this is relevant because society spends a great deal more on old people than it does on younger people. In the UK, the NHS estimate that an 80-year old man is 6-7 times more expensive to the public healthcare system than a man in his 30s. As the size of the elderly population will grow explosively over the next 10-20 years, so will healthcare spending.
Apart from the US, the average OECD country spends about 10% of GDP on healthcare. Only the US deviates meaningfully from that number with healthcare spending in that country being no less than 17% of GDP. Although the numbers in Exhibit 2 below are not measured relative to GDP but are absolute numbers, it is pretty obvious that US healthcare spending is in a league of its own.

Note: 2020 or latest year available
Source: OECD
I have come across one or two ill-informed people who have argued that, of course, the Americans spend more, because the healthcare system is so much more advanced over there, but that is sheer nonsense. If it were so much better, please explain to me why Americans have one of the lowest life expectancies in the OECD.
My point here is not to ridicule the Americans, though. They have chosen a private sector model based on insurance whereas we, in Europe, have chosen a public sector model, based on taxation, and it is every democracy’s right to make that choice. However, when it comes to the cost of it, it is pretty obvious who is on the winning side and who is not.
Disruption - the other megatrend affecting healthcare spending
Changing demographics affect healthcare spending, but it is not the only driver of rising healthcare costs. The accelerating use of various, new and very advanced technologies in the healthcare industry will also impact healthcare spending in the years to come. Most of those new technologies are very expensive, some of them absurdly so, and that will add to healthcare spending.
With the sharp increase in the number of elderly all over the world, one wonders if public healthcare systems can actually afford to take advantage of all those new technologies. In theory, that favours the American model but, in practice (whether in Europe or the USA), only the wealthiest may be able to afford the steep insurance premia which will undoubtedly accompany the new treatment forms, so it is not at all impossible that all those fancy, new technologies will only be used on a small fraction of the populace.
For argument’s sake, let’s assume a solution is found and that, in the years to come, most people will benefit from the forthcoming healthcare technology revolution. That will result in rising life expectancies, as at least some of the new technologies deal effectively with diseases which are deadly today. However, people living longer is expensive for society. In other words, with a tsunami of elderly about to hit public budgets, can society actually afford for people to live longer? It is a terribly cynical question, but it is still a relevant one.
The pros and cons
Many treatment forms have changed in recent years and, if they haven’t, they are about to do so. Take for example the treatment of cancer. For many years, most cancers were treated with a mix of surgery, chemotherapy and radiation therapy. Over the last 15-20 years, targeted therapies – drugs that target cancer cells by homing in on specific molecular changes seen primarily in cancer cells – have become standard treatment forms for many cancers.
More recently, immunotherapy has been added. Immunotherapy is a therapy that enlists and strengthens the power of a patient's immune system to attack tumours. A rapidly growing immunotherapy approach is called Adoptive Cell Transfer (ACT). It collects and uses the patient's own immune cells to treat the cancer. There are several types of ACT therapies but, thus far, the one that has advanced the furthest in clinical development is called CAR T-cell therapy.
According to the National Cancer Institute (see here), CAR T-cell therapy is “… a type of treatment in which a patient's T cells (a type of immune system cell) are changed in the laboratory so they will attack cancer cells. T cells are taken from a patient’s blood. Then the gene for a special receptor that binds to a certain protein on the patient’s cancer cells is added to the T cells in the laboratory. The special receptor is called a chimeric antigen receptor (CAR). Large numbers of the CAR T cells are grown in the laboratory and given to the patient by infusion. CAR T-cell therapy is used to treat certain blood cancers, and it is being studied in the treatment of other types of cancer.”
Until recently, the use of CAR T-cell therapy has been restricted to small clinical trials, mostly in patients with advanced blood cancers. In 2017, two CAR T-cell therapies were approved by the FDA, one for the treatment of children with acute lymphoblastic leukaemia and the other for adults with advanced lymphomas. Although early results are promising, researchers caution that it is still early days for CAR T-cell therapies and other forms of ACT. We do not yet know, for example, whether it is an effective treatment form against solid tumours like breast and colorectal cancer.
I mention this, partially to demonstrate the enormous potential but also to point out the huge cost of it all. Many new treatment forms are excruciatingly expensive. According to Deloitte, 42% of cancer patients in the US have exhausted their savings within two years of diagnosis and, after four years of therapy, 38% are insolvent. This raises a critical question on accessibility. Will everybody be able to access all these new life-saving drugs, or will it be only the (financial) elite who can afford it?
A hidden gem? Not really!
I would probably be guilty of a criminal act, if I suggested that we (Absolute Return Partners) have discovered a hidden gem here. The forthcoming explosive growth in the number of elderly, and the impact it is going to have on healthcare spending, is well advertised. As you can see in Exhibit 3 below, healthcare stocks have significantly outperformed the overall equity market in recent years – at least in the US – and the reason for that is most likely the extraordinarily positive backdrop that I have just referred to.
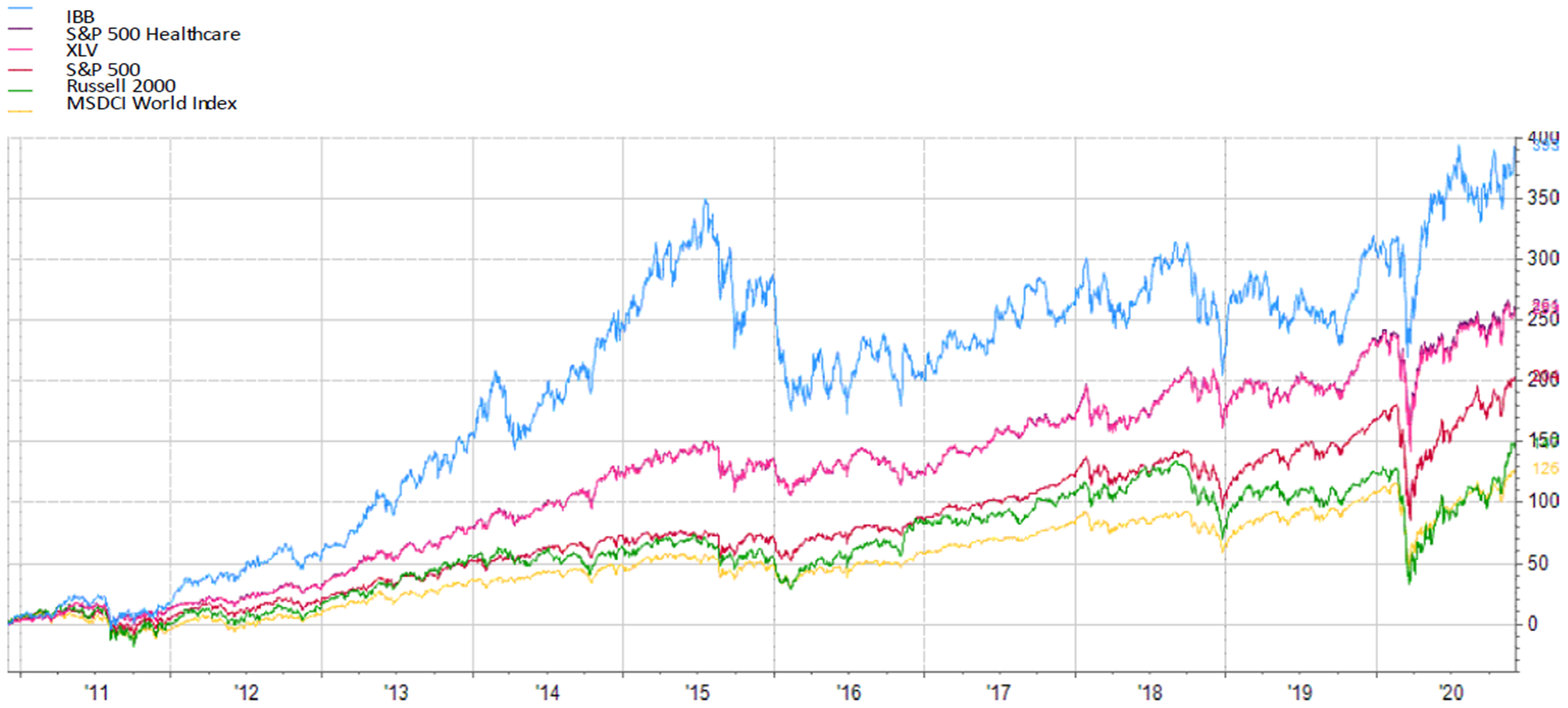
Note: IBB = iShares Biotechnology ETF; XLV = Healthcare Select Sector SPDR Fund.
Source: FactSet, Jefferies Prime Services
This raises the obvious question – are we already too late to the party? For now, suffice to say that, given the escalating number of elderly in most countries, and given the broad array of new healthcare technologies about to be introduced, I don’t think the party is even close to being over.
It may pause for a while if there is a correction in equity markets in general, and one is long overdue, but the combination of ageing of the populace at large and new healthcare technologies/treatment forms could fuel the appetite for healthcare stocks for many years to come.
According to Jefferies, nearly every type of medical expense is on the rise. Although powerful secular trends do not guarantee good investment results, they create robust tailwinds, which investors can take advantage of. CMS projects US national healthcare spending to increase 5.5% annually over the next five years, reaching $5.7Tn or nearly 20% of GDP by 2026.
I should point out that, although demand is growing rapidly, so is supply – of investment opportunities in the healthcare space, that is. According to Morgan Stanley Research, 19 new healthcare companies went public in 2020 on various US stock exchanges, raising a total of almost $8Bn between them. As you can see in Exhibit 4, in the first four months of 2021, another 15 healthcare companies have gone public on US exchanges. This is a powerful indication of the explosive growth in the healthcare industry.
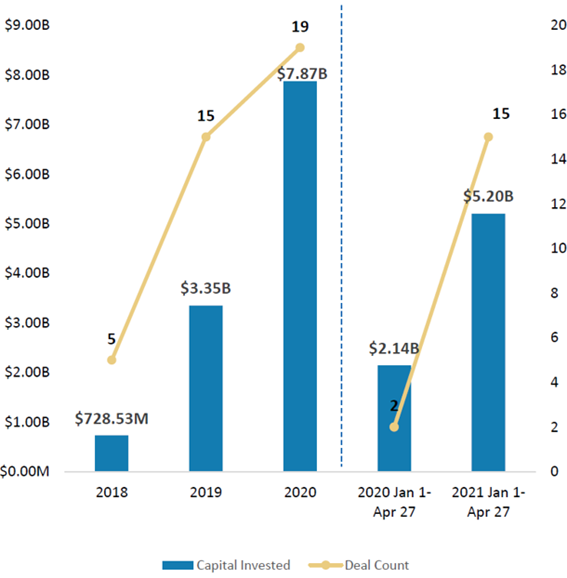
Source: Morgan Stanley Research
Why it is not that simple
Ageing is, contrary to popular belief, a global phenomenon, making the healthcare investment story even better. In fact, in absolute numbers, less developed countries are impacted much more by this trend than more developed countries (Exhibit 5).
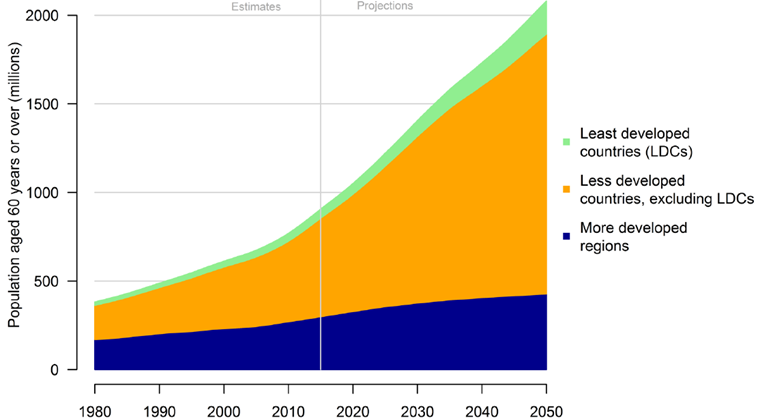
Source: World Population Ageing, UN, 2017
Worldwide, the 60+ age group will grow by about a billion people over the next three decades, and over 50% of that growth will come from Asia (Exhibit 6) – mostly China, I should add. With the 60+ age group growing that dramatically, the healthcare investment opportunity is, at least on paper, massive.
Having said that, public health budgets in many less developed countries may not be sufficient to deal with such steep growth rates. Even in Europe, Northern America and Oceania – regions where the 60+ age group will, between now and 2050, grow by well over 100 million people on a collective basis – affordability may be constrained by already high indebtedness.
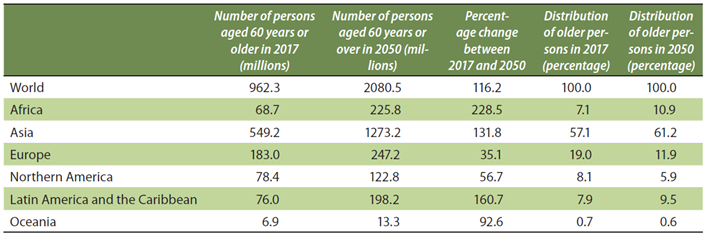
Source: World Population Ageing, UN, 2017
As you can see in Exhibit 7 below, on a percentage basis, Europe is more affected by ageing than any other region. Today, about 25% of all Europeans are 60 or older. By 2030, that number will have risen to 30% and, as you can see, the share of elderly will continue to grow throughout the 2030s and 2040s.
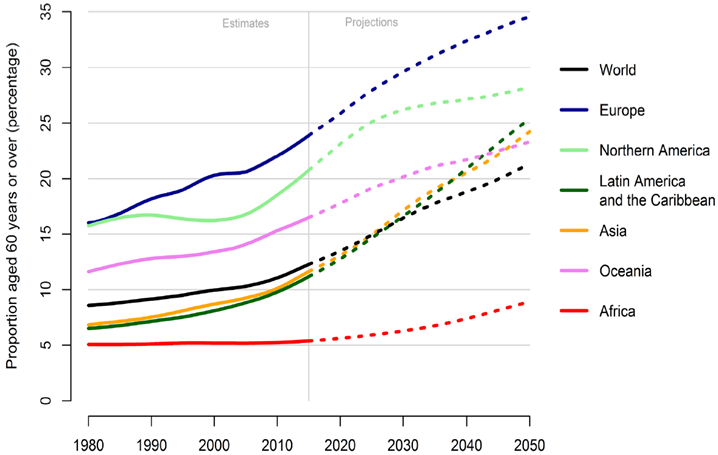
Source: World Population Ageing, UN, 2017
This will put enormous pressure on finances. In less developed countries, the elderly are mostly looked after by their family, but that is rarely the case in Europe (anymore). Therefore, in terms of financial stress symptoms, in more developed countries, and particularly in Europe, one should keep an eye on the public sector, whereas in less developed countries, one should mostly worry about the financial impact on private households.
The population of Europe adds up to about 740 million people so, based on the information provided in Exhibit 7, the 60+ age group in Europe will grow by 35-40 million people over the next decade. The impact on public budgets will be huge. For example, in the UK, the NHS estimates that 55% of its budget is spent on the over 85s (see here).
From an investment point-of-view, provided the European healthcare model doesn’t collapse, this could be a major opportunity, rarely seen bigger, so what is the risk of a collapse? Many European countries are already heavily indebted and may end up struggling with the oncoming tsunami but, as we have all learned in recent years (from Japan), as long as interest rates are under control (read, sufficiently manipulated), public indebtedness can be almost infinite.
Another important lesson has been learnt in recent years, and that is that most politicians these days are populists. As long as old people continue to vote – and, in most countries, the elderly use their right to vote more vigorously than younger people do – politicians will increasingly deliver what the elderly want/demand, even if the country in question cannot afford it.
Adding it all up
Simply put, there is one overriding question that all investors will have to deal with:
Is the old-age tsunami an outstanding investment opportunity, or will it slow down economic activity to a trickle and potentially even bankrupt entire countries, making the investment environment rather tricky?
The short answer to that question is “probably a little bit of both”. Let me explain by going back to the UK example, but I wouldn’t expect other developed countries to show a markedly different picture. As you can see in Exhibit 8 below, healthcare spending per person is relatively stable until people reach the middle-ages; however, once they reach the age of 50, healthcare spending increases, and the increase in spending continues to accelerate until the show is ultimately over.

Source: The Guardian, The Nuffield Trust.
If you combine the facts that (i) 55% of the NHS budget is spent on the approx. 1.6 million people who are aged 85 or older, (ii) the 85+ age group is expected to almost double over the next decade, and (iii) the UK government is already quite indebted, it doesn’t take a genius to figure out that it could face massive financial problems.
In that context, I should point out, that the demographic outlook in the UK is not that bad – far superior to the outlook in Germany, Italy and Spain. In other words, if the UK could end up in financial trouble, what about, say, Italy? The country is already drowning in debt and is facing dramatically inferior demographic statistics.
Having said that, while I still think there is a big investment opportunity lining up here, it is because the old will dictate the agenda in most democracies in the years to come, and most governments will be able to afford it, as long as they are prepared to (continue to) manipulate interest rates.
Enjoy your otium!
Niels C. Jensen
1 September 2021
Membership required
Membership is now required to use this feature. To learn more:
View Membership BenefitsSponsored Content
Upcoming Virtual Events View All